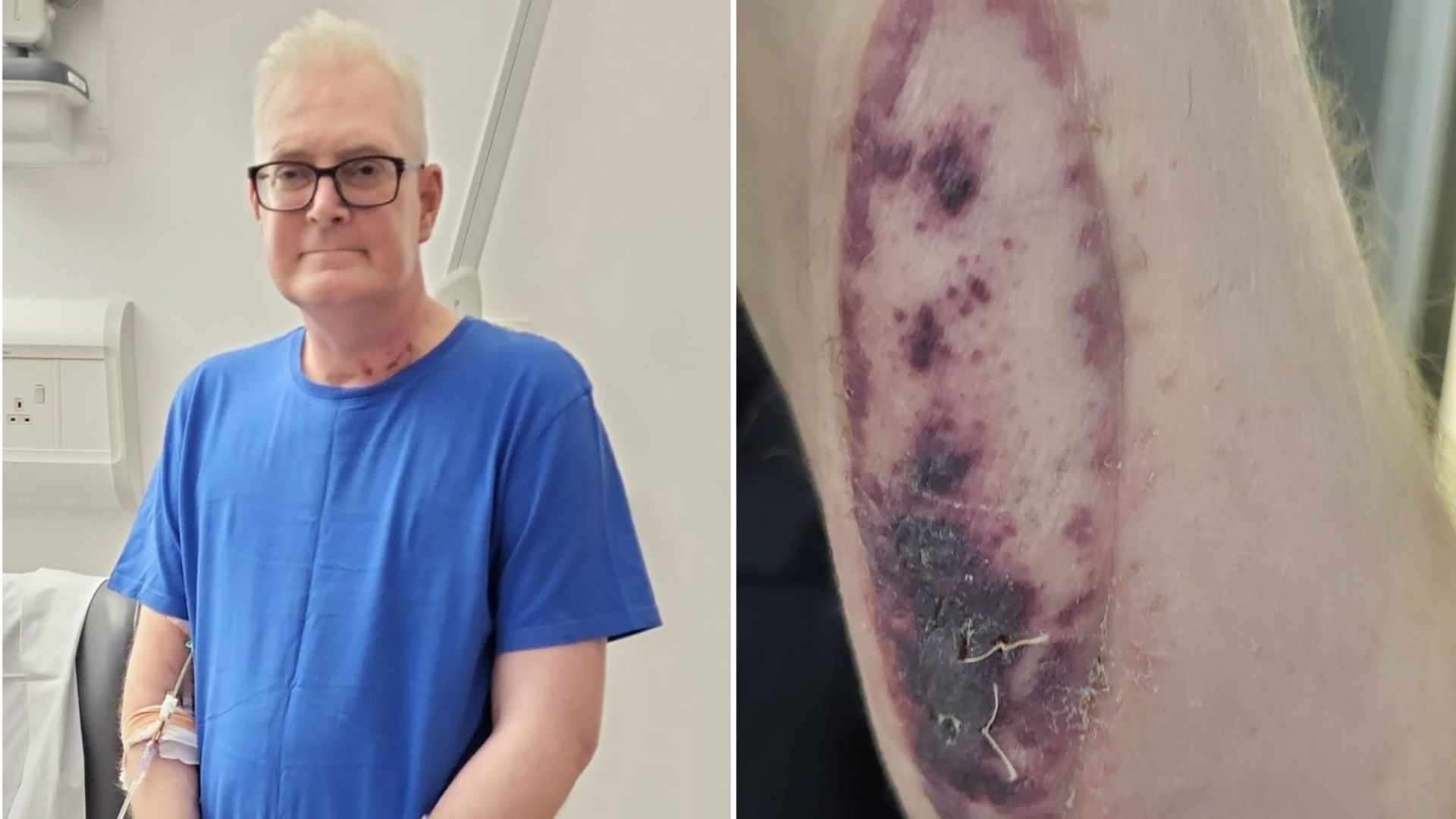
Medical miracles don't always look like high-tech scanners or glowing screens. Sometimes, they look like a small, unassuming square of skin. Recently, a lung transplant recipient discovered that their body was rejecting a new organ not through a lab result or a sudden cough, but by looking at a "sentinel" skin patch. It’s a brilliant bit of surgical foresight. When we think about organ transplants, we usually focus on the internal plumbing—the veins, the arteries, and the heavy lifting of the heart or lungs. We forget that the immune system is a silent, aggressive guard dog. It doesn't like strangers.
The skin patch technique involves grafting a small piece of the donor’s skin onto the recipient's forearm at the same time as the primary organ transplant. Because skin is one of the most immunologically active tissues in the body, it reacts to rejection faster than an internal organ often does. If that patch starts looking red, bumpy, or irritated, it's a visual alarm bell. It tells the doctors that the body is gearing up for a fight before the new lung even starts to fail. If you liked this article, you should read: this related article.
The Brutal Reality of Lung Transplant Rejection
Lungs are notoriously difficult to transplant. They're delicate. They're constantly exposed to the outside world through the air we breathe, making them prone to infection and inflammation. Statistics from the International Society for Heart and Lung Transplantation show that nearly 50% of lung transplant recipients experience some form of rejection within the first five years. That’s a staggering, scary number.
Traditional monitoring is a bit of a nightmare for the patient. You’re looking at frequent bronchoscopies, where doctors shove a camera down your throat to snip off bits of lung tissue for a biopsy. It’s invasive. It’s uncomfortable. It carries its own risks of bleeding or lung collapse. Worst of all, by the time a biopsy shows damage, the rejection process is already well underway. You’re playing catch-up with your own immune system. For another perspective on this story, see the recent coverage from Healthline.
The sentinel skin flap changes that timeline. It gives a visible, external window into what’s happening inside. Think of it as a smoke detector. You’d rather see a tiny flickering light in the hallway than wait until the kitchen is actually on fire. That’s exactly what happened in this recent case. The patient noticed changes in the donor skin patch on their arm. They didn't feel sick yet. Their breathing hadn't tanked. But that skin was screaming for help.
Why the Skin Acts as an Immune Early Warning System
Our skin is our primary barrier against the world. Because of this, it’s packed with specialized immune cells like Langerhans cells. These cells are basically the scouts of the immune system. When you transplant a piece of donor skin, you’re putting those scouts on the front line.
Researchers at institutions like Oxford University and the University of Pennsylvania have been championing this "sentinel" concept for years, though it’s still not the standard for every hospital. The logic is sound. Skin is more "antigenic" than many internal organs. This means the immune system notices it faster and attacks it more visibly.
When the recipient's T-cells—the "assassin" cells of the immune system—identify the donor tissue as foreign, they swarm the area. In a lung, this causes microscopic damage that eventually leads to scarring and breathing failure. On the arm, it causes a rash. I’d take a rash over lung failure any day. This visual cue allows doctors to tweak immunosuppressant dosages immediately. They can stop the attack before it scars the lung tissue, which is often irreversible.
Beyond Lungs and Into Multi Organ Cases
This isn't just about lungs. We're seeing this technique used in complex "VCA" or Vascularized Composite Allotransplants. Think face transplants or hand transplants. In those cases, the skin is already part of the package. But for internal organs like the liver, kidney, or lung, adding a separate skin patch is a conscious, strategic choice by the surgical team.
It’s about more than just detecting rejection. It’s about peace of mind. Imagine being a transplant survivor. Every time you have a slight tickle in your throat or feel a bit tired, you wonder. Is this it? Is my body rejecting the gift I was given? Having a physical marker you can check in the mirror provides a level of psychological control that shouldn't be underestimated.
The Surgery Behind the Patch
It’s not just a simple "peel and stick" job. The surgeon has to perform a microvascular procedure. They take a small section of skin from the donor—usually from the abdominal area—along with its underlying blood vessels. They then plumb those vessels into the recipient’s arm.
This ensures the skin patch has its own dedicated blood supply. If it was just a surface graft, it wouldn't accurately reflect the systemic immune response. It has to be "alive" and connected to the patient’s circulatory system. This is a highly technical skill. It adds time to the surgery. It adds another incision site. But the payoff is a 24/7 monitoring system that doesn't require a hospital stay or a needle in the chest.
Common Misconceptions About Transplant Monitoring
People think that if their blood work is fine, their organ is fine. That’s a dangerous assumption. Lab markers like creatinine for kidneys or oxygen saturation for lungs are "lagging indicators." They tell you what has already happened. They don't tell you what is currently brewing.
The skin patch is a "leading indicator."
- Visual cues happen first. Redness or swelling at the graft site often precedes internal organ dysfunction by days or even weeks.
- Biopsies are easier. If a doctor needs to confirm rejection, they can biopsy the arm patch. It’s a simple "punch" biopsy that takes five minutes and a Band-Aid. No sedation. No risk of punctured lungs.
- Personalized medicine. Every patient processes anti-rejection meds differently. The patch helps doctors find the "Goldilocks" zone—just enough medication to protect the organ, but not so much that it destroys the kidneys or leaves the patient open to deadly infections.
Challenges and Limitations of the Sentinel Flap
Let's be real. It isn't a perfect system. Not every donor is a candidate, and not every recipient wants a patch of skin on their arm that might look different from their own. There’s a cosmetic element here. The donor skin might have a different tone or texture. It’s a permanent scar.
There's also the rare risk of "isolated rejection." Sometimes the skin patch rejects but the organ is fine, or vice versa. While rare, it can lead to "false alarms" that cause unnecessary stress. However, in the vast majority of documented cases, the correlation between the skin and the organ is remarkably high. Doctors generally agree that a false alarm is better than a missed one.
What You Should Ask Your Transplant Team
If you or a loved one are on a transplant waiting list, you need to be your own advocate. Most centers won't offer a sentinel skin patch unless you ask or if they are part of a specific clinical trial. It’s still considered "innovative" rather than "standard of care" in many regions.
Ask about their monitoring protocols. Ask how they handle "silent" rejection. Mention the skin patch technique specifically. Some surgeons might find it unnecessary, but others might be willing to bring in a plastic surgery specialist to make it happen. You want every tool in the shed when your life is on the line.
The success of this recent lung patient isn't just a feel-good story. It’s a call to action for the medical community to move toward more proactive, visible monitoring. We have the technology to sew tiny blood vessels together. We should use that skill to give patients a way to see their own health.
If you're heading into a transplant, don't just focus on the surgery day. Focus on the years after. Demand the tools that make those years safer. Pay attention to your body, and if your team offers a way to make the invisible visible, take it. Keep an eye on your skin. It might just be the thing that keeps you breathing.